Medicine in Medellin: The National Health Care System (Part Two)
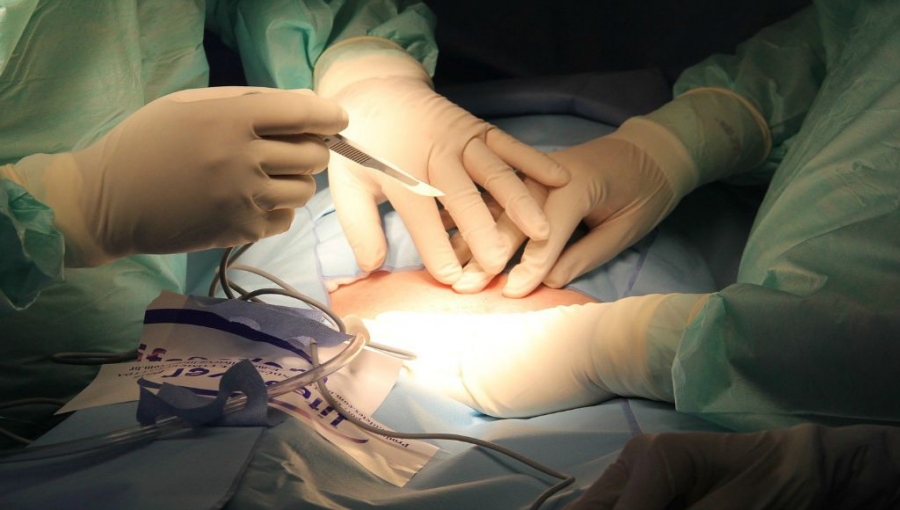
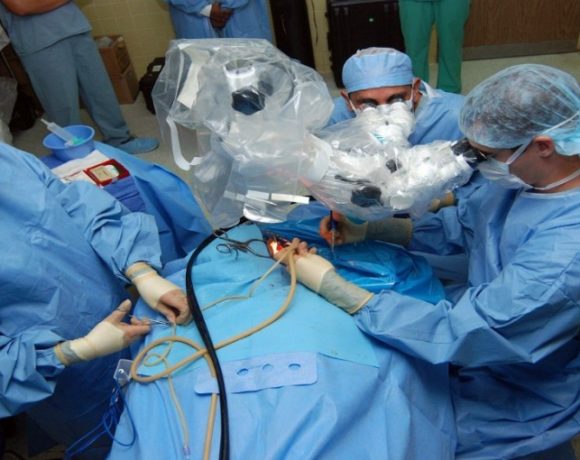
Medical tourism is a growing business for metro Medellin thanks to an international reputation for high quality, high technology, friendly service and competitive prices.
But in contrast to this encouraging news for medical tourists – those mainly in the upper-end private sectors — most of the recent news stories about medical care in Medellin specifically and in Colombia generally have focused on the national health-system financing crisis.
This is of special concern to the vast majority of Colombians — as well as resident expats and tourists lacking cash or foreign insurance who don’t qualify for (or can’t afford) Colombian private, pre-paid health insurance, or else lack resources to pay cash-for-services, whenever the need may arise.
However, this public financing crisis won’t affect medical tourists coming to Medellin through the private Salud Sin Fronteras (SSF) network, as these SSF patients will have already pre-qualified for ability-to-pay via letters of credit and other means (see “Medicine in Medellin, Part One”).
On the other hand, those living here with thinner wallets must rely upon the mostly under-funded public hospitals, some private clinics, and the public or private “EPS” (entidad promotora de salud) networks – roughly similar to the health maintenance organization (HMO) networks in the United States.
This financial crisis is slamming hospitals, clinics, and remaining EPS health networks, some of which have gone out-of-business in recent years or else have been converted into mixed public-private entities, such as the giant Savia Salud EPS that now covers a large portion of Medellin and Antioquia populations.
What’s more, a growing number of private clinics now flatly refuse to attend patients affiliated with certain EPS networks that are vastly in arrears on bill payments.
National, state and local treasuries likewise are overwhelmed with enormous health-care bills originating from services to millions of mainly low-income Colombians that pay little or nothing for health insurance, medical procedures or medicines.
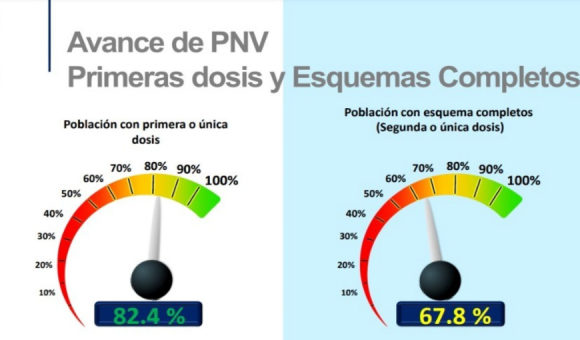
According to the most recent government statistics, per-capita spending on health care in Colombia is less than US$500 per year – just 7% of the per-capita health-care spending in the U.S.
But even if Colombia had the most efficient public-health system in the world – which critics say is far from the actual situation – the per-capita spending still wouldn’t be nearly enough to cover the costs, according to many experts.
On a nationwide basis, the EPS network organizers, hospitals and clinics today have hundreds of millions of dollars of unpaid and overdue bills, mainly thanks to recent court decisions and recent Colombian Congress legislation that declares that all Colombians have a “right” to health care — even if they don’t pay anything, or pay relatively little.
This situation is likely to get worse before it gets better, thanks to the “new health statute” (Nueva Estatuaria de Salud) law that was passed in early 2015, according to experts.
Problem: The new law doesn’t automatically guarantee that Colombia will devise better, smarter, cost-effective regulation and operation of public health services, or require smarter cost/benefit decisions, or mandate national tax hikes that could pay for the huge increase in services.
Meanwhile, Colombia’s Health Minister Alejandro Gaviria has publicly suggested the idea of a new tax on sugary beverages, to boost health-system revenues. But the Congress – facing elections this fall — has yet to move on any new tax legislation to shore-up the health system.
Such health services could become even more expensive in future as hospitals upgrade equipment, boost medical-staff training and obtain stricter certifications, according to experts.
Demographic changes – that is, Colombia’s growing proportion of older citizens – also could impose even greater burdens on under-funded health services.
In the meantime, some Colombian hospitals are so far behind in paying their own vendors – such as those who wash hospital laundry, maintain the surgical equipment, replace the light bulbs and so-on – that they’re shutting-down (or threatening to shut-down) certain wards that don’t at least break-even on costs, with maternity wards being a prime example.
Other hospitals in Colombia are so far behind in paying their employees — sometimes for six months or more– that street demonstrations have erupted. In other cases, some hospitals have closed entirely, while others say they’re teetering on the brink.
‘Contributory,’ ‘Subsidized’ Regimes
Millions of Colombians – including those that have “informal” rather than regular jobs — don’t contribute any money to the national system. They fall into the vastly under-funded “subsidized” regime.
Millions of others who have “regular” jobs are in the “contributory” regime, putting part of their paychecks into the national system, while employers contribute another part. Some of this “contributory” money gets diverted to cover medical expenses of those in the “subsidized” regime.
A third sector – the “pre-paid,” private-sector regime – is funded entirely by relatively well-off Colombians who pay vastly more for health insurance (or else just pay in cash) than either the “contributory” or “subsidized” sectors.
These patients sometimes don’t have to wait as long for certain emergency services, and these patients typically enjoy faster approvals for certain medicines and specialist procedures — since hospitals and doctors don’t have to worry about getting paid by relatively stable, well-financed, “pre-paid” insurance service organizations.
Under the current regulatory scheme, the EPS organizations are supposed to ensure that their hospital and clinic networks provide a specified list of mandatory services and medications (“POS” or “Plan Obligatorio de Salud”) at certain government-dictated prices.
For those patients lacking pre-paid insurance or lacking sufficient cash, obtaining services that fall outside the POS list still can be mandated via individual patient lawsuits (“tutelas”).
Problem: Government funds to cover “non-POS” services are vastly short, leaving EPS networks and hospitals on-the-hook for unpaid services.
Law 100 Debate
Prior to 1993, when the Colombian Congress passed Law 100 (Ley 100), the bulk of the Colombian population didn’t have any constitutional right to health care. Instead, patients could pay in cash (if they were wealthy enough), beg for hospital or doctor charity, or else buy private insurance.
Since then, a series of laws, reforms and health-network entities have arisen, with the result that 97% of Colombians now have “access” to health care, at least on paper.
But for many of those in the EPS network systems, this “access” is often accompanied by lengthy service delays; standing in lines to get prior approvals for certain exams, tests or medicines; denial-of-service for certain costly procedures, and denial of access to certain costly medicines and specialists.
Because the clinics, the EPS organizations and the government haven’t been able to cover the growing demand for services from people who put little or no money into the system, hundreds of thousands of “tutelas” have swamped the Colombian court system — creating lots of work for lawyers and judges, and wasting money that might better be spent on a more-rational national health system.
On the up-side, people in the pre-paid system – as well as those medical tourists using the SSF private network of hospitals and clinics — wouldn’t face these headaches.
However, for much of the rest of the Colombian population, better-funded, better-managed and more-rational health-care system solutions have yet to be formulated and implemented.
Next/Part Three/Experts Debate National Solutions